Dialysis is the process of removing waste and excess water from the blood and is used primarily to provide an artificial replacement for lost kidney function in people with renal failure. Dialysis is regarded as a life sustaining measure until a renal transplant (Kidney transplant) can be performed, or sometimes as the only supportive measure in those for whom a transplant would be inappropriate.
Dialysis is needed when one has end stage kidney failure or CKD V, usually by that time loss of about 85 to 90 percent of kidney function is seen and have a GFR of <15. And if patient has severe symptoms caused by kidney disease, such as: shortness of breath, fatigue, muscle cramps, nausea or vomiting or biochemical abnormalities like very high urea, creatinine, potassium or acidosis.
When kidneys fail, dialysis keeps body in balance by:
Usually yes, but not always. The chances that the kidneys will get better depend on what caused kidney failure. Kidney failure is divided into two general categories, acute and chronic. Acute (or sudden) kidney failure is often temporary. Some kinds of acute kidney failure get better after treatment. In some cases of acute kidney failure, dialysis may only be needed for a short time until the kidneys get better. In chronic kidney failure, the kidneys normally do not heal and may require lifelong dialysis or they can get transplanted.
Dialysis can be done in a hospital (hemodialysis) in the dialysis unit. Patients usually have hemodialysis three times a week. It takes about 4 hours each time.
Dialysis can be done at home (peritoneal Dialysis). Patients perform the peritoneal fluid exchange by themselves or with the help of a relative ate home.
In hemodialysis, the patient's blood is pumped through the blood compartment of a dialyzer, exposing it to a partially permeable membrane. The dialyzer is composed of thousands of tiny synthetic hollow fibers. The fiber wall acts as the semipermeable membrane. Blood flows through the fibers, dialysis solution flows around the outside of the fibers, and water and wastes move between these two solutions. The cleansed blood is then returned via the circuit back to the body. Ultrafiltration occurs by increasing the hydrostatic pressure across the dialyzer membrane. This usually is done by applying a negative pressure to the dialysate compartment of the dialyzer. This pressure gradient causes water and dissolved solutes to move from blood to dialysate, and allows the removal of several liters of excess fluid during a typical 4 hour treatment. It is usually done thrice weekly.
Hemodialysis requires a strict treatment schedule, regular medications and usually, changes in the diet.
Dialysis can be done in a hospital (hemodialysis) in the dialysis unit. Patients usually have hemodialysis three times a week. It takes about 4 hours for each session.
In hemodialysis, an artificial kidney (hemodialyser) is used to remove waste and extra chemicals and fluid from blood. Before the first dialysis treatment, an access is surgically created to get blood from the body into the hemodialyser and is returned to the body. This is typically a quick operation and will allow patient to return home the same day.
Usually, an access is made by joining an artery to a vein under your skin to make a bigger blood vessel called a fistula.
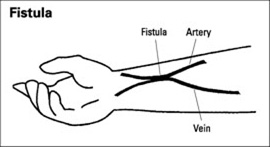
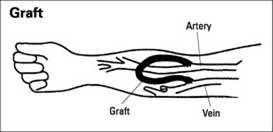
However, if your blood vessels are not adequate for a fistula, a PTFE tube is used to join an artery and a vein under your skin. This is called a graft.
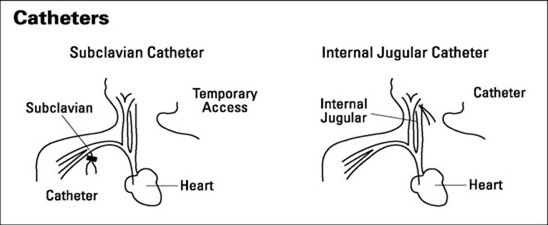
Occasionally, an access is made by means of a narrow plastic tube, called a catheter, which is inserted into a large vein in your neck. It is most commonly used as a temporary access when someone needs dialysis immediately or when they are waiting for a fistula/graft to mature. This type of access may be temporary, but is sometimes used for long-term treatment.
Avoid all pressure on the access site. If the graft or fistula clots, you may need a new one.
Do not miss or skip any dialysis sessions. Make sure time is maintained as the dialysis units are busy with regular schedules.
Dialysis carries several risks, although many can be avoided through proper procedure and careful use of equipment. Risks associated with dialysis include:
A dialysis nurse can train patients to perform home hemodialysis. Patients do not have to buy a machine. Supplies can be delivered. Both the patient and any caregivers must learn to:
In peritoneal dialysis, a sterile solution containing glucose is run through a tube into the peritoneal cavity, the abdominal body cavity around the intestine, where the peritoneal membrane acts as a partially permeable membrane. The peritoneal membrane or peritoneum is a layer of tissue containing blood vessels that lines and surrounds the peritoneal, or abdominal, cavity and the internal abdominal organs (stomach, spleen, liver, and intestines). The dialysate is left there for a period of time to absorb waste products, and then it is drained out through the tube and discarded.
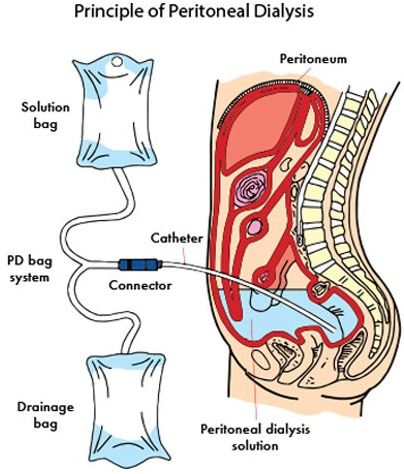
This cycle or "exchange" is normally repeated 3 - 5 times during the day, (sometimes more often overnight with an automated system). Each time the dialysate fills and empties from the abdomen is called one exchange. During the dwell time (means the time of dialysate stay in patient's abdominal cavity) wastes, chemicals and extra fluid move from patient's blood to the dialysate across the peritoneum. A drain process is the process after the dwell time, the dialysate full of waste products and extra fluid is drained out of patient's blood. Ultrafiltration occurs via osmosis; the dialysis solution used contains a high concentration of glucose, and the resulting osmotic pressure causes fluid to move from the blood into the dialysate. As a result, more fluid is drained than was instilled. Peritoneal dialysis is less efficient than hemodialysis, but because it is carried out for a longer period of time the net effect in terms of removal of waste products and of salt and water are similar to hemodialysis. Peritoneal dialysis is carried out at home by the patient. There are two types of peritoneal dialysis……
Although support is helpful, it is not essential. It frees patients from the routine of having to go to a dialysis clinic on a fixed schedule multiple times per week, and it can be done while travelling with a minimum of specialized equipment.
Good and highly efficient dialysis depends, not only on the machine or the technician, but more so on the quality & purity of water supplied to the machine. A patient is exposed to an average of 120 liters of water in a dialysis session of four hours. Hence the water supplied to the patient should be of the purest quality.
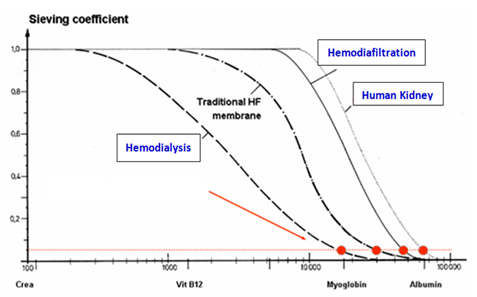
In the traditional hemodialysis, a maximum of 4 liters of water is removed from the body along with accumulated toxins. This is performed by a process called diffusion. The traditional hemodialysis machines have a single revolving blood pump. The hemodialysis machine can clear toxic molecules only up to 600 – 2000 daltons in size. The human kidney can clear toxic molecules up to 120,000 daltons in size. Hemodialysis needs dialysis grade water.
With the latest technical advances, and the availability of ultrapure water, a process called hemodiafiltration is now possible. In Hemodiafiltration up to 48 liters of ultrapure water are sent into and simultaneously removed from the patient in a four hour session. This results in highly enhanced clearance of toxins. This process combines both convection and diffusion and thus is vastly superior in toxin removal. Hemodiafiltration can clear up to 60,000 daltons, thus closely replicating normal kidney function.
The graph below illustrates the superiority of hemodiafiltration over hemodialysis and its close replication of human kidney’s clearance of molecules of increasing sizes.